Hello All,
I left off in the last post with April just getting her PICC line. After her PICC line, April’s NG tube was still producing a lot of bile and she was still extremely nauseous. April, even with the NG tube in place and sucking out the contents of her stomach, was still having moments of vomiting. The night was a fairly long one with her vomiting and gagging, and now in pain from the NG tube and her pain in her back and abdomen went up from all the vomiting and retching. When I tried to close my eyes it was about 1 am and she had another 850ml in her NG canister. April woke up throughout the night, it was just a bad night.
The next morning our accustomed hospital regiment started. At 6am the colorectal resident rounded, then at 6:15 the spine team rounded and then around 7 the pain resident rounded. At 8am the attending colorectal physician rounded. I spoke with him and told him I was concerned about another obstruction, however unlikely it may be, but that I was still concerned. He acknowledged my concern, but did not think she was completely blocked up and had an ileus and that the NG tube will help. He was confident her bowels just needed a little longer than normal to get going again because of everything she has been through, and that I completely agreed with.
A couple hours after the attending physician left, April’s physical therapist and occupational therapist came together for a session. Even though April has been put through the ringer and was up all night in pain and retching, she was game to try to do anything. She was able to get to a sitting position, stand, do some marching in place and take a few steps forward and back, all of this with her back brace and help from the therapist. Sitting may seem like a mundane event in our lives, but it is an absolute chore and takes a lot of strength for a person with a fused spine, especially after surgery. It is a little hard to explain so here is a quick YouTube video of what April has to do just to sit, and mind you she also had her abdomen opened up about 7 inches so her abdominal muscles are in pain as well. Video
After April’s physical therapy session there was a change in color and consistency to what was being sucked out of her stomach. Instead of the green liquid bile there was now reddish brown liquid with clumps of “stuff” in it. On occasion there were little streaks of red. I was little concerned because of the red color, especially since she has been getting Lovenox (a blood thinner) injections since she has been in the hospital so long and they worry about blood clots. I was concerned of an abdominal bleed. The nurse paged the doctor and he came down and looked and spoke with me. The chunks were a mixture of blood clots from her bowel surgery and part of the ileus. So it was a good sign the ileus was getting decompressed. As a precaution we changed the canister out to a new one so we could get a better visual of what was coming out. April was still producing a lot of fluid into the canister. About 600ml in the canister in a 6 hour period.
In the evening the pain doctors came on through and suggested that April get a Fentanyl patch since April had been doing well on the Fentanyl PCA. About 9pm the TPN finally arrived and I was very happy to see it. This will give her some protein and fats and electrolytes, so finally after 11 days her body will get some nutrition. April slept a little better through the night, her nausea had settled down and the NG was still producing fluids but it had slowed down a little.
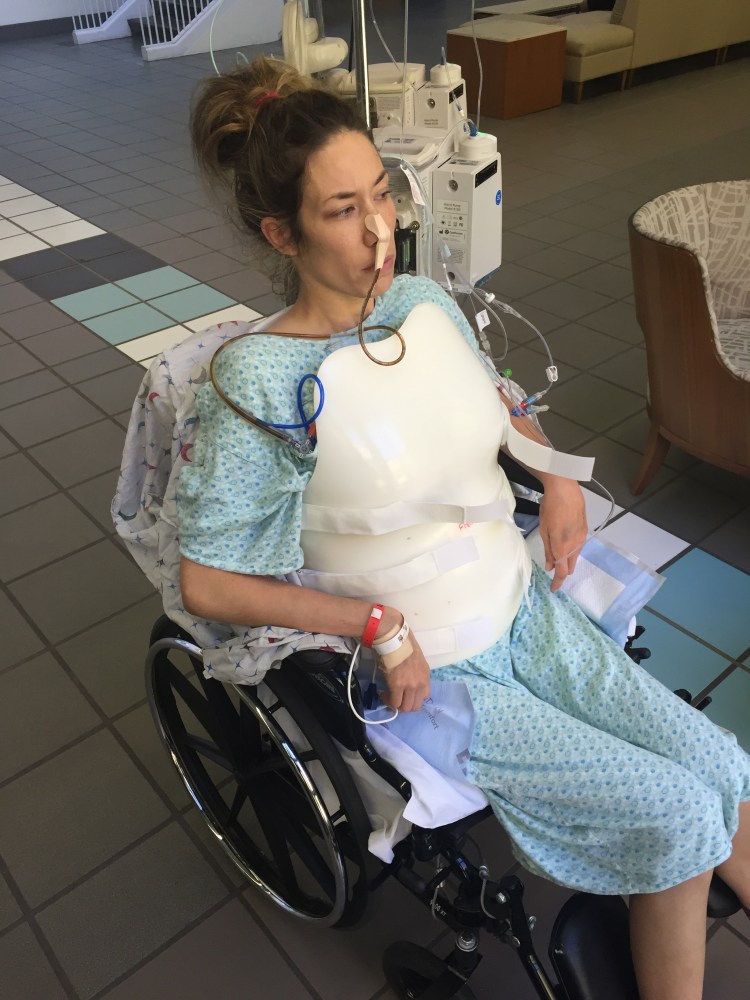
You can see how much weight she has lost
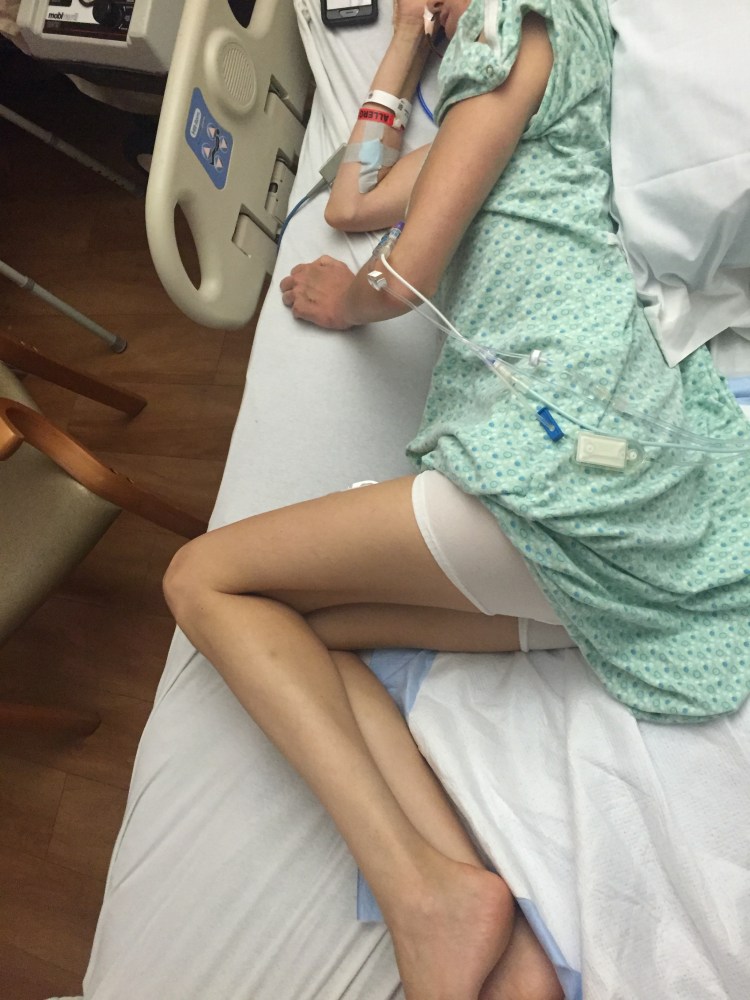
In the morning the routine began again. The colorectal residents rounded on her and said they are taking things slow, so still nothing to drink or eat, which we were totally fine with after the the past few days of bile vomiting. Her output had slowed quite a bit over the night and the color was now a light green so this was a good sign. About an hour later the attending colorectal physician, as well as the Chief surgeon, came to talk to us. It is amazing the attention you start to get when everything has gone wrong. Well, they came and talked with us about clamping off April’s NG tube for a 4 hour trial period to see how her stomach does and see how much gastric output she will have. April’s nurse came in to clamp off the NG tube and also told her the doctors ordered her to have her urinary catheter taken out. April was not thrilled about her catheter coming out because she can’t even walk so how is she supposed to get to the bathroom. I told her not to worry you get to use a bedside commode, something every woman loves to hear.
Speaking of the commode, an hour after her urinary catheter was taken out April was able to try it out. Now this may be very strange for most people to talk about, unless they work in the medical field or have had surgery, but April had an actual BM. And yes, this was very exciting and very important. This meant that April’s bowels were finally beginning to work in the correct direction.
After this momentous occasion came another milestone. April had her PT session and walked the length of the hall. This was way further than she had walked before so this was a big deal. She started to feel real tired and weak so we put her in the wheel chair and wheeled her back to her room, but she did some great work. Having said that, there has been no improvement in her left leg. April still can’t feel it and she has no idea what it is doing or where it going, but she is able to use a walker and walk a little ways. Her ballet training has definitely helped her with walking because she has a very good ability of visualizing her body in her mind. So when she walks she is literally thinking about how her leg and foot look in her head and how they should move. She can’t feel the ground or how high she is lifting her leg, but because of her strong body awareness she is at least able to “walk.”
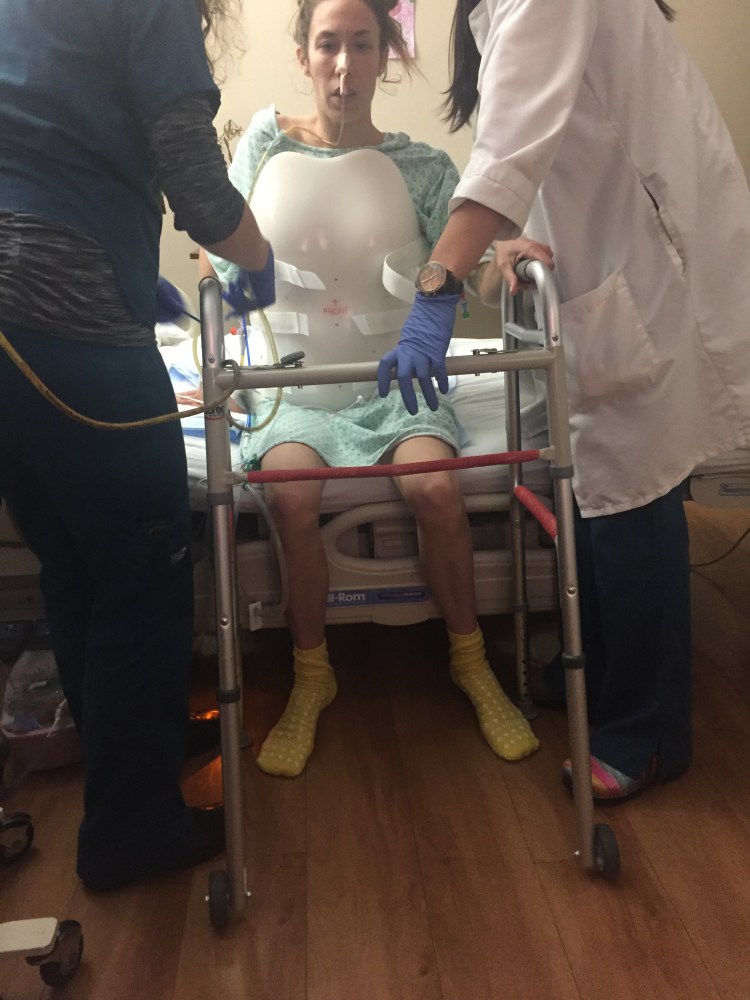
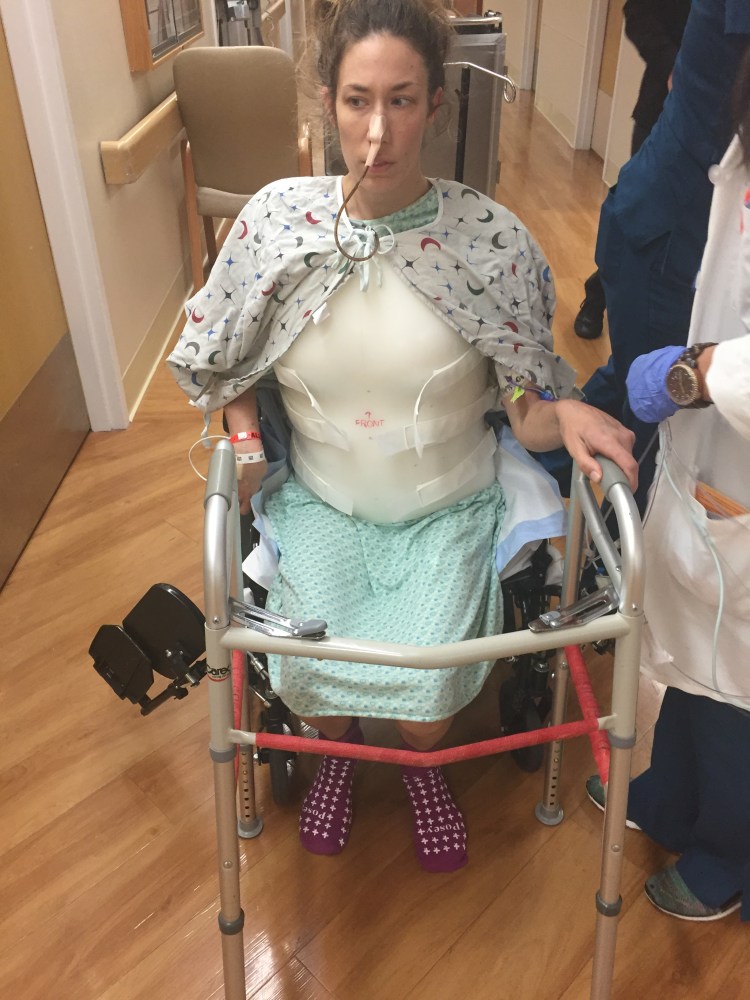
After April’s PT she was wiped out and it was time for the nurse to check the output of her stomach. They hooked her NG back up to suction and only about 60ml came out which was great. The doctors wanted to do another 4 hour trial just be cautious and if her about was the same or less her NG could come out. In the next 4 hours April was able to use the commode multiple times, again I know kind of gross, but highly important. For her to use the commode it is like equivalent to her PT sessions because she has to log roll to the side of the bed, push up keeping everything straight and as her upper body goes up her legs must come down to the floor. Then she has to get to her feet, then to the walker, then back into the commode. When she is done, then it’s back up to the walker, over to the bed and lay correctly then log roll over to the middle. So including her huge PT session she did like 8 or 9 smaller PT sessions. By the evening she was hurting pretty bad and every muscle was having spasms.
After the 2nd 4 hour NG trial was over the nurse could only pull out 30ml of fluid and it was more of a clear fluid. The doctor went ahead and told the nurse to pull out the NG tube, but that April was still not allowed to eat or drink, he wanted to wait through the night. Around 9:30pm April’s new TPN came and it was double the size of her one from the previous night. I was very happy to see it because she has just lost so much weight and this will help her muscles and body get some nutrition. April slept a little better this night, mostly because I think her body was just depleted of any energy. In the middle of the night she needed to use the bathroom and she couldn’t even stand. Her poor body has been through a lot and last night it was done.
Pain meds and TPN

This morning, once again, the routine: the colorectal doctors rounded, then the spine doctors, and then the pain doctors. The colorectal doctors told us April can now have some ice chips and clear liquids. The spine doctors changed her dressing and her incision looked dry. The pain doctors just wanted to see how her pain management was going and that they wanted to keep her on IV pain management a little while longer until her stomach has tolerated real food. Sounded like a good plan to us.
I had to basically force April to eat some ice chips. She is just so gun shy about eating anything right now and I told her I understand, but no way to get better until we start with this. She finally ate some and had some water with no problems, so the doctors bumped her up to the next stage which is chicken noodle soup and popsicles and things like that.
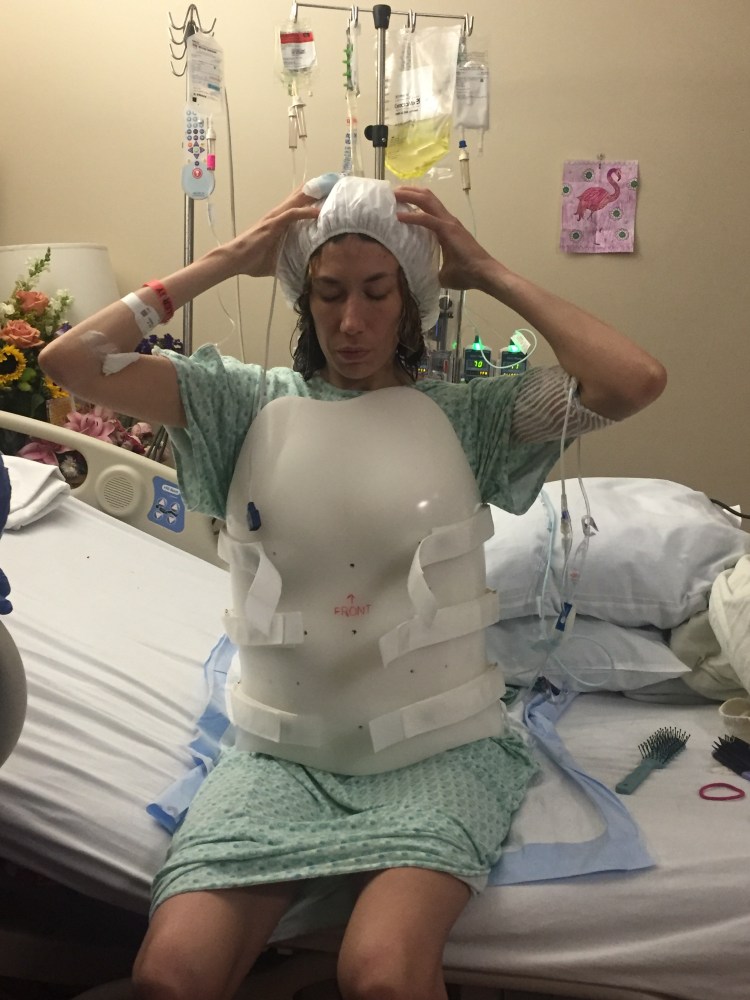
April a little bit ago was able to wash her hair wth the occupational therapist. They used a shampoo shower cap, so it wasn’t like a real washing, but nonetheless I could tell she felt better after getting all the knots out and having clean hair. The physical therapist came in right after and did a low key session for April since she could barely move from all of the moving around yesterday. As much progress that she has made in the past few days with her bowels and beginning to eat, April is ever so cognizant of her left leg. She couldn’t help but breakdown with the therapist because she just can’t do anything on her own, not even stand. I try to refocus her on the positive and tell her one step at a time: 1st we need to get your body eating food and get you strong babe and get you moving, then we will worry about that leg. It is definitely On my mind constantly, but we have to focus on what she needs at this minute, in order to get us to the next minute and so on.
Learning to do some everyday things with a new back


A brief ride in the wheel chair to look at the garden


Woohoo! So much goodness in this post! Thank you for the update. I wish I were closer so I could bring her a plastic champagne flute for her ice chips! She’s a classy lady and deserves some sophistication for her ice. 😉 I think she looks beautiful with her hair in a nice clean bun. I bet getting cleaned up felt great. I hope you’re feeling good, too, Neil. You’re doing an important job of advocating for her as s encouraging her. The left leg will take time but I’m confident it’ll come around.
LikeLiked by 1 person
Dearest Neil and April,
Step by step, one function at a time April is healing. I am very much in admiration for your couple dynamic. Before the surgery the love April has for you was perspiring in each words she wrote in her blog about you. And now that it is you who is writing I can read all the love you have for every cell of her body, any spark of her soul in your careful description of your days and nights after the surgery. You two are an inspiration for me, a vivid image of what love looks like between a husband and a wife. Blessed are you two!
I keep praying for April to heal and for you Neil to keep your hope strong.
LikeLiked by 2 people
So very happy to hear good news! I’m glad positive steps are happening for April!!
LikeLiked by 1 person
This post brought me to happy tears. Any progress is amazing and I’m so happy you had a few days of progress instead of setbacks.
LikeLiked by 1 person
Neil – thank you for sharing the updates! I know this is extremely hard on you and your family – but please know you have more people than you could ever imagine sending positive thoughts your way! Keep up your hard work – we know April will keep up hers!! We will continue to send our positive thoughts and prayers your way!!
LikeLiked by 2 people
Hugs- so glad to hear more good news…and thank you for the truth here…we used to joke that surgical patients are the only people who get very happy and excited about farts and BMs. But…when they are NOT happening, it is big trouble. Hoping for some peaceful sleep for both of you.
LikeLiked by 2 people
so glad to hear she is making forward progress. Stay strong.
LikeLiked by 1 person
Having had spinal and other surgery and worked in surgery I know where you are coming from. Great progress and I’m glad the TPN is flowing. You are doing an amazing job!
Aprils colour looks better in the latter photos. Hair wash is as good as any medicine too.
Keep it going April. My thoughts are with you and your amazing family. Xxx
LikeLiked by 1 person
She is doing amazing, she is a strong woman… I had surgery for scoliosis 2 years ago and sitting is horrid… After surgery i had high heart rate, blood transfusion and severe leg pain in my left leg… It took about 7 weeks for my leg to get better, but they was no answer to what was causing it.. They now say think is just muscle pain… I still have nerve damage around my hips and feels weird to touch as some places are really sensitive and other areas numb… I watch everyday for updates on april and so nice to see… She as been through so much and is so lucky to have someone like you supporting her every step of the way…
LikeLiked by 1 person
Positive thoughts . I put her on our a prayer list
LikeLiked by 1 person
April is amazing! My thoughts and prayers are with her and your family.
LikeLiked by 1 person